Our history
From cholera in the Victorian East End to AIDS in the 1980s, from the streets of today's London to HIV overseas - Mildmay has always walked towards the crisis others turned away from.
This is that story.
1866: The Calling
Mildmay’s story starts in the 1850s and 60s with The Reverend William and Catherine Pennefather – vicar of St Judes and St Paul’s Church in Mildmay Grove, Islington, who, together, had developed a number of projects known collectively as Mildmay Institutions, providing spiritual guidance and care for the sick.
In 1866, Cholera was raging unchecked through the rookeries of the Old Nichol - one of the most notorious slums in nineteenth-century London, a tangle of twenty narrow streets where 6,000 people lived in 730 crumbling houses, and where even the police would not go alone. Death carts rumbled through the streets all night.
Two Mildmay Deaconesses, trained in nursing by Catherine, volunteered to go into the Old Nichol to care for the sick and their dependents. The cholera epidemic eventually burnt itself out, but the Deaconesses kept coming, every day, to Bethnal Green. The principle had been established: Mildmay goes where the need is greatest.

'St Jude and St Paul's, Mildmay Grove - William Pennefather's church, and the name behind the 2024 Mildmay line. It was a lively Victorian church of over 1,000 people in Pennefather's day and still plays an active and important part in its local community.

1877: The First Mission
Victorian photograph of Cabbage Court in the Old Nichol slums, Bethnal Green.

Charles Booth coloured the Old Nichol in black - the lowest of his scale, denoting the most deprived area. The location of the 1977 Mildmay Mission (black) and 1892 Hospital (green) is marked.

The Old Nichol was situated between Shoreditch High Street and Bethnal Green Road. It consisted of 20 narrow streets containing 730 dilapidated terraced houses which were inhabited by some 6,000 people.
By 1877 the work had outgrown its informal roots.
William had died in 1873, and Catherine, carrying the mission forward in his memory, opened the first Mildmay Medical Mission in a converted warehouse in Cabbage Court (now Bacon Street), in the heart of the Old Nichol. It had twenty-seven beds across three wards, one doctor, three nurses, and five deaconesses in training.
The hospital asked no letters of admission and turned no one away on grounds of faith, though prayers were said on the wards and biblical verses painted on the walls. In practice, it became a lifeline for the large Jewish immigrant community in the East End, a remarkable detail given the fervently evangelical Christian ethos that underpinned it. The Mildmay Medical Mission was formally recognised as a nurse training institution in 1883, one of the first in the country.
In the 1880s and 1890s, the London County Council cleared the Old Nichol as part of the Bethnal Green Improvement Scheme, replacing the slums with the Boundary Estate, the first social housing development built by a local authority anywhere in England. The rubble of the demolished slums was used to build the elevated bandstand at the centre of Arnold Circus, which stands to this day.

Arnold Circus on the Boundary Estate, built on the rubble of the Old Nichol slums. The bandstand is yet to be completed

The Boundary Estate today (Arnold Circus)

1892: A Purpose-Built Hospital
With the Old Nichol facing demolition, a new location was chosen: Austin Street, on the corner of Hackney Road in Bethnal Green.
A foundation stone was laid in 1890, and in 1892, the first purpose-built Mildmay Mission Hospital opened its doors with fifty beds in three wards: male, female, and children.
Emily Goodwin became its first Matron. The hospital clock, mounted above the main entrance in 1892, survives to this day above the entrance to the current hospital, one of the few physical artefacts connecting the two buildings across more than a century.

Emily Goodwin, first Matron of Mildmay Mission Hospital, 1892.

The main entrance portico of the 1892 hospital

The hospital clock survives to this day above the entrance to the current hospital
1914–1945: Through Two Wars
Mildmay served its community through both World Wars.
During the First World War, the hospital continued treating the sick of Bethnal Green while the wider health system was strained to breaking point by casualties from the Western Front. During the Second World War, the hospital remained open through the Blitz, when the East End was among the most heavily bombed areas of London.

Mildmay during the Second World War
A 1938 fundraising booklet, 'The Hospital with a Difference', records a visit by Queen Mary and gives a vivid picture of the institution in its pre-NHS years: a community anchor, drawing support from local businesses, churches, and donors of all backgrounds. The adverts in its pages, from paint suppliers to laundry services, hint at the hospital's deep -rooted place in local East End life.

The Hospital with a Difference - Mildmay's 1938 fundraising booklet, featuring a visit by Queen Mary

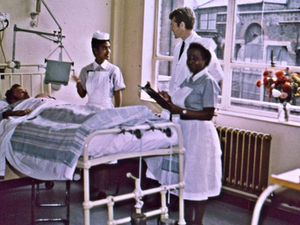
Christmas at Mildmay, Children's Ward, c.1949
1948: Joining the NHS

Anenurin Bevan, Minister of Health, on the first day of the National Health Service, 5 July 1948 at Park Hospital, Davyhulme, near Manchester.
(Image credit). Right: NHS information as reported at the time

On 5 July 1948, the National Health Service came into being.
With the creation of the NHS in 1948, Britain introduced the world’s first comprehensive, tax-funded national health service, free at the point of use for everyone, regardless of means. It was a transformation in the relationship between the state and its people that had no peacetime precedent.
Mildmay joined the NHS that year, incorporated into the North East Metropolitan Regional Board's Central Group of Hospitals. It transferred to the East London Group in 1966, and in 1974 became part of the Tower Hamlets Health District. For the next three decades, Mildmay operated as an NHS hospital, continuing to train nurses and serve the community of the East End.

A Mildmay nurse training certificate from 1951

1982–1985: Closure and the Fight to Survive
Mildmay and its staff before closure - a hospital that had served its community for over a century
But the economics of the NHS were not kind to small hospitals.
By 1980, as a 'cottage hospital' with fewer than 200 beds, Mildmay was deemed uneconomic. The process of running it down began in the early 1980s.
In January 1983, more than 400 supporters marched from Mildmay Hospital to Trafalgar Square in protest at the decision to close it. It was the kind of gesture that rarely changes minds in Whitehall, but Mildmay's supporters, led by the extraordinary Helen Taylor Thompson, Chair of the Trustee Board, refused to give up.
Kenneth Clarke, then Minister for Health, agreed. In May 1985 he announced in Parliament that Mildmay would reopen outside the NHS, as a voluntary charitable hospital, on a long-term lease at a peppercorn rent.
In October 1985, the doors opened again. A thanksgiving service was held at St Paul's Cathedral.
There followed two years of meetings, proposals, setbacks, and legal argument. The decisive moment came when Peter Frymann, advising the Hospital Advisory Council, pointed out a clause in the 1948 National Health Services Act: the Minister of Health was legally responsible for maintaining the denominational character of hospitals where that was appropriate. Mildmay was one of only six hospitals covered by this provision. Closing it, the argument ran, was not maintaining anything.

1988: Europe's First AIDS Hospice
Diana, Princess of Wales, arriving at Mildmay Hospital, East London
In 1988, the government asked Mildmay to do something that almost no one else was willing to do: care for people dying of AIDS.
At the height of the epidemic, fear and stigma around the condition were overwhelming. Some healthcare workers refused to treat patients. Families were sometimes too frightened to visit their dying relatives. AIDS was understood to be caused by a virus, HIV, but public understanding was limited, misinformation was rampant, and the disease carried a weight of social shame that compounded the suffering of those who had it.
Princess Alexandra officially reopened the hospital on 19 May 1988 as Europe's first dedicated AIDS hospice. The wards were renamed; the mission was reborn. A converted residential care centre, Spencer House, was added as a family unit, the first residential family care facility in the world for people with HIV/AIDS and their loved ones.

Princess Alexandra officially opened Europe’s first AIDS hospice at Mildmay Hospital in 1988.

Nursing Times article covering the official opening.

Mildmay's Spencer House Family Care Centre
Then came Diana
Diana, Princess of Wales, made seventeen visits to Mildmay between 1989 and 1997 - three official, fourteen unofficial, sometimes arriving at eleven at night and staying into the early hours. She would sit with dying patients, hold their hands, and talk.
In April 1987, at a separate event, she had shaken hands with an AIDS patient in front of the cameras, a gesture that reverberated around the world at a time when many believed the virus could be transmitted by touch. At Mildmay, she did it again and again, in private, without cameras, because she wanted to.

Diana with nurses and care staff at Mildmay

Diana in conversation with families

Princess Diana's foreword to the book, A Time to Care - Mildmay Hospital's response to people with AIDS, by Ruth Sims.
The press coverage of Diana's visits helped to shift public understanding of AIDS in Britain in ways that no public health campaign could have achieved alone. Within ten years of its closure by the NHS, Mildmay was cited in Hansard as the model of care for people with AIDS in the UK.

An article about Mildmay from the East End Life newspaper, May 1995.
1996: A New Kind of Hospital

'The Brain Impairment Nursing Team, 1997. Mildmay's early specialisation in HIV-related neurocognitive disorder
In 1996, the introduction of highly active antiretroviral therapy (HAART) - three-drug combinations that could suppress HIV to undetectable levels - transformed the landscape.
AIDS was no longer a death sentence for most patients with access to treatment. Deaths from AIDS in the UK fell by 80% between 1995 and 2000.
The hospice became a rehabilitation centre. Patients who had arrived expecting to die were leaving, sometimes slowly, sometimes against expectations, to live. By 2008-09, there were just two deaths at the hospital in a single year. Two-thirds of patients were going from what medical staff called 'death's door' back to life in the community.
Mildmay developed particular expertise in HIV-associated neurocognitive disorder (HAND) - the effect of HIV on the brain, which can cause patients to lose the ability to walk, speak, or feed themselves.
Today, Mildmay is the only specialist HAND rehabilitation unit in Europe. This is the work that defines the hospital now: not end-of-life care, but the painstaking, skilled work of helping people reclaim their lives.
1993 onwards: Going Global
From 1993, as HIV was devastating communities across sub-Saharan Africa, Mildmay was called to extend its expertise beyond London.
Projects were established in Uganda, Tanzania, Kenya, Zimbabwe, Rwanda, and later Eastern Europe, sharing the knowledge accumulated during the AIDS crisis years with health systems in some of the worst-affected countries in the world.
In Uganda, this grew into something lasting. Mildmay Uganda Hospital was formally opened in 1998 by the Princess Royal, and over the following decade developed into an independent institution encompassing a hospital, research centre, and a school of health sciences. In 2007, Queen Elizabeth II visited the hospital and its paediatric care centre, a recognition of how far the work had come.
Over the years, these projects have been handed over to local organisations with the capacity to sustain them. In 2024, Mildmay International was wound down, and Mildmay Kenya transferred to full independence under its own Board of Trustees.
Our focus now is on sharing expertise through local partnerships rather than running programmes directly. For example, the Education Exchange Programme sends UK clinicians to Uganda to gain field experience in resource-limited settings that strengthens their practice and, in turn, the NHS, and in 2026, we launched the ambitious Uganda Health Programme.
'Mildmay's international work began in the 1990s, starting in Uganda and extending across sub-Saharan Africa

Queen Elizabeth II visitng Mildmay Uganda in 2007

2014: A New Hospital, the Same Mission
The current Mildmay Hospital, opened September 2014, built within the footprint of the original Victorian building.
In 2011, the 1892 building was demolished.
What replaced it was something purpose-built for the twenty-first century: a new specialist HIV hospital, opened in September 2014, constructed within the footprint of the old Victorian building on the same Shoreditch site. The hospital clock from 1892, which had hung above every generation of Mildmay's main entrance, was remounted above the new one.

The 1892 hospital clock, restored and mounted above the entrance to the new Mildmay Hospital.
The new building was designed from the ground up around the needs of patients with complex, long-term conditions , with single en-suite rooms rather than open wards, spaces for the multidisciplinary therapeutic work that defines modern rehabilitation, and an environment that felt less like an institution and more like a place of recovery. The two inpatient wards were named Catherine and William, after the Pennefathers. The mission they founded in 1866 had found a building that matched it.
In December 2015, Prince Harry officially opened the hospital and cut the anniversary cake to mark the start of Mildmay's 150th anniversary celebrations - a moment of public recognition for an institution that had spent over a century earning its place as one of London's most quietly remarkable hospitals.

Prince Harry officially opens the new hospital, December 2015, as Mildmay begins its 150th anniversary year
Timelapse video of the demolition of the old Mildmay Mission Hospital buildings in 2011.

2020: The Pandemic and a New Purpose
PPE stocks at Mildmay Hospital during the COVID-19 pandemic, 2020
In 2020, COVID-19 brought the NHS to the edge of its capacity.
As acute hospitals across London strained under the surge in admissions, the pressure to free up beds became urgent. Mildmay was asked to help and responded by becoming London's primary referral unit for homeless patients with COVID-19 who needed non-intensive inpatient care.
Out of that emergency came something lasting. The Step-Down Homeless Medical Care Pathway, the first of its kind in London, was built on a simple and urgent principle: patients recovering from illness or injury but with no home to return to were being discharged from acute hospitals back onto the streets. Mildmay provided the bridge. A clinical environment where they could recover properly, with medical care, therapy, and the support needed to move on. The Care Quality Commission recognised it as an area of outstanding practice in its 2021 inspection.
As the pandemic receded, the need did not. In 2022, Mildmay launched the REBUILD Pathway, specialist inpatient care for homeless patients who had undergone detoxification from alcohol or drugs, but who needed time, support, and a stable environment to consolidate their recovery before returning to the community.
Patients receive nursing, medical, and therapeutic care in a psychologically informed setting, alongside housing
and discharge planning. The goal is not just physical stabilisation. It is the kind of sustained, human support that makes the difference between someone returning to the streets or beginning a new chapter.
The same years have seen Mildmay working with NHS England and the Department of Health, aiming to develop new rehabilitation pathways, extending the specialist expertise in HIV-associated neurocognitive disorder that has defined the hospital's clinical identity for three decades.
It is, in its way, the same instinct that brought two women in crinolines into the Old Nichol in 1866: go where the need is greatest.

Mildmay senior nurses Teri and Comfort with a new EEG machine in 2022.

2024: The Mildmay line

TfL's 2024 naming honours the hospital's place in East London history.
In February 2024, Transport for London announced that one of six newly named London Overground lines would be called the Mildmay line, running between Stratford and Richmond and Clapham Junction, and marked on the Tube map in blue.
The naming was proposed in recognition of Mildmay Hospital's pioneering care for people with HIV and AIDS during the 1980s and 1990s, its long history of serving the people of East London, and its continuing significance to the LGBTQ+ community today.
The line officially launched in November 2024. Every day, hundreds of thousands of people travel the Mildmay line - many without knowing the name's origin. But it is, quietly, one of the most significant acts of public recognition the hospital has ever received.

Mildmay line signage at Stratford station.

2025 marked forty years since Kenneth Clarke announced in Parliament that the hospital would live again, and the doors opened in October 1985 to begin a new chapter that none of those involved could fully have anticipated.
2025: Mildmay at 40
The year-long anniversary celebration culminated in a reception bringing together former chief executives, staff past and present, trustees, patrons, clinicians, partners, and friends, a gathering that captured the scale of what Mildmay has become.
The occasion also marked two further milestones: Mildmay’s rehabilitation centre was named in honour of Lord Fowler; and Lord Smith of Finsbury was welcomed as the hospital’s new President.
The naming of the centre after Lord Fowler carries its own historical weight. As Secretary of State for Health and Social Services under Margaret Thatcher from 1981 to 1987, Norman Fowler was the driving political force behind the UK’s response to AIDS, fighting within a sceptical Cabinet to launch the “Don’t Die of Ignorance” campaign in 1986, which sent a leaflet to every home in Britain and shocked the country into confronting a crisis it had preferred to ignore. Thatcher reportedly told him he risked becoming known as “the Minister for AIDS” and that she disapproved; Fowler pressed on regardless. His conviction that AIDS was a public health issue, not a moral one, helped shift the terms of public debate at a moment when that shift could save lives.
It was under his tenure that Mildmay’s AIDS work was authorised and supported.
His junior minister, Kenneth Clarke, was handling the direct negotiations over the hospital’s lease. Forty years on, the rehabilitation centre that bears his name treats patients recovering from exactly the kind of HIV-related complications that Fowler’s campaign helped bring into public view. It is a fitting connection.
Forty years on, the mission has not changed. The conditions have. HIV is no longer a death sentence. Homelessness and addiction are the new crises that bring people to Mildmay's doors. The hospital that was once told it had no place in the modern NHS is now the model; for complex HIV rehabilitation, for homeless step-down care, for post-detox recovery. It remains the only specialist HIV rehabilitation unit in Europe.

CEO Geoff Coleman with Lord Fowler and Lord Smith

From the archive
Mildmay holds a remarkable photographic archive spanning more than a century - some of it rescued, literally, from a skip.
The man who saved it was Bert Miller, a porter and volunteer at the hospital for thirty years, whose own life story is inseparable from Mildmay's history.
Bert lived through both world wars, survived the Blitz, and spent decades caring for patients at a time when the NHS was still finding its feet. When the hospital began clearing out old storage rooms in the 1980s, Bert saw what was being thrown away: glass plates, prints, albums, and he intervened. His daughter has since told his story, and the photographs he saved now form the heart of Mildmay's visual memory.

Bert was a keen photographer